Integrated Acute Care: The Impact of a Patient Centered Admission Team
When patient care is a priority, there is a natural integration of more and more elements of the patient’s hospital experience, from their entry process through their stay and finally their discharge. Not only is integrating care delivery service more efficient at delivering care – it’s more effective.
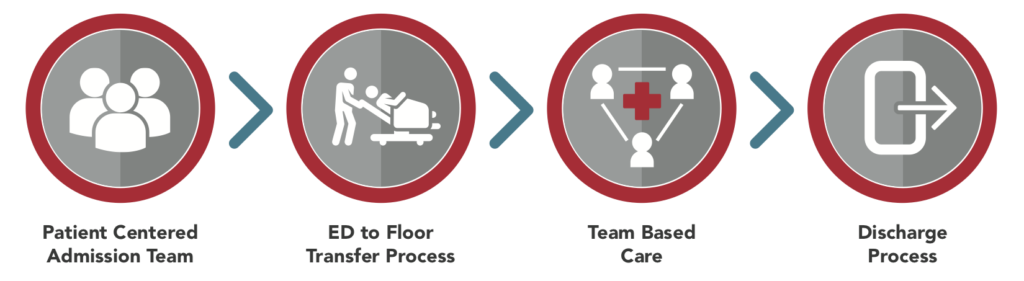
An integrated care delivery model starts with the process of admission, then the quick and efficient transfer of the patient, seamless, efficient delivery of care to the patient, and an equally smooth discharge process. The following image demonstrates the key components of this integrated care delivery model.
This all sounds very simple. But in reality it is quite complex, with a multitude of moving parts, departmental hand-offs, documents to track and people to keep informed and engaged. There are a variety of models in existence, each suited to the size, volume, complexity and infrastructure of different healthcare institutions. We will walk through a model designed for a large, multi-specialty organization with very high patient volume. These hospitals often depend on efficient patient processing in order to provide bed capacity. Not every hospital is like this, however. Some very small facilities might find that this particular model is too costly to initiate and maintain.
However, some form of integrated care, for any healthcare organization, can have a huge impact. Rapid admission processing and nursing assessment, error-free patient care and medication delivery and efficient processes such as medication reconciliation can profoundly reduce Length of Stay (LOS), drop readmission rates and raise patient satisfaction scores. Better management of patient evaluations and assessments also helps reduce costs by enabling more efficient work-load rebalancing. If the hospital can better understand patient needs, during more of their stay, it can more accurately assess staffing needs, too.
This article will primarily cover the impact of a Patient Centered Admission Team.
The PCAT (Patient Centered Admission Team)
In most hospitals, admissions are processed by a number of different providers acting independently of one another in a sequential order, often resulting in delays, errors, redundancy of effort, higher costs and lower patient satisfaction. Sequential processing requires that things be done in a very rigid manner to produce the lowest error rate. A well-known example of this is in the airline industry, where pilots go through a very rigid checklist prior to departure every single time. Healthcare is full of sequential processes, and for good reason, in most cases. An example would be the checklist process prior to surgery, in which, similar to an airline pilot, the surgeon follows a checklist to ensure he has the right patient, the correct surgical procedure on the correct side and so on. I myself recently underwent surgery on my tongue and they actually marked the outside of my left cheek since that was the side the surgery was going to be on. Obviously, I’m glad the sequential process helped ensure my surgery was error-free, even though the process took time and resources to complete.
Parallel processing on the other hand is geared for efficiency. Multiple things can be done at the same time. Anyone who takes their car to an oil change shop can see a good example. While one person is taking your information, another is draining the oil and a third is under the hood checking fluid levels. Your car is in and out much faster than if you’d changed the oil yourself, in a sequential order of tasks.
There aren’t many parallel processes used in healthcare because the multiple individuals involved work in separate, siloed environments. Pharmacists have their own process, as do ED nurses, physicians, technicians, and every other healthcare professional. Rarely do they work together in parallel. However, The PCAT process is a parallel process specifically designed to improve care delivery and efficiency in the healthcare system.
Regardless of admission type and portal of entry, the admission process will typically involve the following providers, each of whom is responsible for a portion of every admission:
- Physician: history and physical, orders
- Nurse: nursing assessment, medication delivery
- Pharmacist: medication reconciliation, medication review, order review, MAR
- Technician: vital sign acquisition, weight, transport set-up, blood draw, EKG
The patient must wait for each task to be completed, one after the other, and hope that none of the providers or departments involved is having a heavy workload that day. Any delays cause the entire process to delay. Before instituting a PCAT, we measure the standard approach to admissions. The following are actual findings from such a study:
- Full history & physical: 25 minutes
- Full admission orders: 5 minutes
- Head to toe nursing assessment: 60 minutes
- Medication reconciliation: 15 minutes (varies depending on who completes)
- Production of an MAR: 180 minutes
- Dispense medications: 60 minutes
- Report and handoff to floor nurse: 10 minutes
- Report and handoff to floor provider: 10 minutes
Standard Admission Time = 6 hours and 5 minutes
Placing the provider required for admission on a special PCAT team, all of whom are in one place, has a profound effect on performance and patient care. This PCAT team, working in parallel and able to coordinate each person involved in the patient’s care delivery, can immediately provide a complete work-up of the patient. Ongoing care can be provided immediately, with no re-work, no error and no delay. With every component of an admission completed on the spot, the patient is launched smoothly into the system. This approach is quicker, results in fewer errors, improves efficiency and also boosts patient satisfaction scores.
PCAT Admission Time = 50 minutes
Patients processed by the PCAT team take on average 50 minutes from notification to completion of an MAR. This process time includes the exact same tasks as are currently performed by providers to admit a patient.
Some patients, particularly those requiring immediate intervention and disposition, such as STEMIs or unstable surgical patients, will need to be managed wherever their immediate needs land them in the hospital. These non-ED portals of entry can provide their own highly coordinated teams and processes for streamlining admissions, similar to the PCAT.
The admission process for patients will vary depending on their portal of entry to the hospital:
- Elective surgical admissions are predominantly worked up weeks to months in advance. These comprise the majority of surgical admits.
- Direct admissions to the hospital are often similar to elective surgical cases but with a much shorter timeframe. They often come, for example, from a Primary Care Provider (PCP) with a History & Physical examination (H&P) and orders written.
- Elective Cath Lab patients are handled in the same manner as surgical cases.
- Transfer patients are usually managed similar to ED admissions.
- ED admissions can average upwards of 45% of all hospital admissions. These patients come in a variety of types:
- ICU—these patients’ lives are in immediate danger. The ICU therefore requires the highest level of care and the fastest admission and transfer.
- Surgical or Cath Lab—also requiring quick admission and transfer, these patients are managed by the surgical or cardiac team. Patient disposition status is determined after the procedure.
- Observation—Outpatient status patients requiring a stay in the hospital.
- Inpatients—these patients have been reviewed and meet inpatient criteria for a hospital stay.
The volume of admissions per PCAT team is usually 1 per hour. The number of teams necessary to process any given ED’s patients can easily be calculated. Take for example an ED that admits an average of 30 patients per day, with fluctuations from 20 to 40. To manage 30 patients per day requires 3 teams on 8 hour shifts, plus an overlap team for busy periods for a team capacity of 32 patients per 24 hour period. Contingency plans must also be considered for those days when volumes exceed this capability.
Concerns are likely to be raised regarding team costs. However, workload re-balancing should result in the teams being fairly cost neutral. Workload re-balancing is simply moving staff assignments to meet needs within the organization. An example of this would be to reduce nursing staff on the hospital floor to reflect a reduction in the need of nursing hours there. Because the PCAT team performs nursing assessments up front, there is no longer a need for nurses on the hospital floor to perform this hour-long task per patient. A PCAT team that processes 30 nursing assessments a day has removed 30 hours of nursing assessment workload from the hospital floor. Reallocating those nursing hours to the PCAT team is more efficient and does not raise costs.
Each member of a PCAT team can similarly be rebalanced. The pharmacist on the PCAT team, for example, significantly reduces intra-pharmacy workloads by performing order entry and MAR tasks up front. This enables a reallocation of pharmacists at no additional cost to the organization – while improving operational efficiency and quality of care.
Physician workload does not significantly change. But the physician’s time is spent more efficiently, and he is better positioned to deliver quality care in a timely fashion to his patients.
PCAT location
In organizations with plenty of empty bed capacity and no delays in bed assignment or transfer of patients from the ED to hospital beds, a roving team should be able to provide the PCAT assessment on the unit. High volume, capacity constricted hospitals, with extended boarder hours in the emergency department and delays in patient flow will require an ED based model. This allows for the process to initiate immediately once the decision to hospitalize an ED patient has been made.
Real-World Impact
In a PCAT system, care delivery begins immediately following the request for hospitalization. This is extremely important in many disease processes which demand ongoing aggressive care. Patients awaiting admission can deteriorate, resulting in longer lengths of stay, increased complications and increased costs, aside from the obvious increase in danger and discomfort to the patient. CHF, COPD, Asthma, Dehydration, Hyper or Hypoglycemia and Urgent Hypertension are just a few examples of conditions requiring speedy admission and immediate care.
PCAT patients also move through the complex hospital system more smoothly and efficiently. They already have a full nursing assessment and their initial medications when they arrive on the hospital floor, which has several key benefits. Floor nurses need not be pulled for extensive periods from other patients, and there is far less chance for medication error. And long wait times for drugs to be delivered are heavily reduced. A recent study, excerpted below with the author’s permission, provides excellent data on the impact of a PCAT implementation in practice.
Abstract Patient Centered Admissions Team (PCAT): Value of a Decentralized Pharmacist in a Multidisciplinary and Patient-Centered Team in Improving Patient Flow in the Hospital
Award for Excellence in Medication‐Use System 2012 Application Patnawon Thung, PharmD
Primary Impact 1—Reduction in processing time from admission to MAR completion:
Primary Impact 2-Accuracy of Medication—Use of a pharmacist in completing medication reconciliation at the time of admission results in significant interventions and is able to identify medication list errors patients carry on a regular basis. Accuracy of medication reconciliation of medications at the time of admission for 190 cases over 9 weeks follows:
To shed some light on what these numbers really mean, consider just the 94 medication corrections that were made at the time of the PCAT team evaluation. Under standard circumstances this would have resulted in 94 phone calls being made by the pharmacist to the provider to correct the medication error. That’s a lot of provider time if you consider a phone call to be even 1 minute, and that every call was answered immediately. That’s over 1.5 hours correcting medications. Time that could be spent caring for patients.
This clearly demonstrates the significant impact a pharmacist can have on medication reconciliation at the time of admission.
Primary Impact 3—Pharmacy intervention in Drug information, Drug interaction, Dosage adjustments, Pharmacokinetics, Substitutions and over volume of orders entered per week follows:
These types of interventions are not only cost effective but profoundly impact patient safety and proper drug utilization. This also demonstrates how workloads are rebalanced. With these orders and interventions now being carried out at the bedside by a pharmacist in real time, the workload of the central pharmacist, who previously performed these tasks in a central pharmacy, is decreased. Moving these tasks to the bedside is clearly safer for the patient, and is more cost-efficient for the hospital, too.
Secondary impacts were found to be significant when comparing PCAT patients to the same patient types admitted by the pre-PCAT methodology.
Secondary Impact 1- Length of Stay
This finding supports the theory that providing care to patients more quickly results in more rapid recovery and an earlier discharge. Patients with many disease processes such as asthma, congestive heart failure and hyperglycemia require aggressive initial therapy and uninterrupted treatment, even as they move through the system. Patients with co-morbid conditions such as hypertension require regular medication, or else they may experience worsening of their untreated co-morbid condition. These types of cases are reflected in this data.
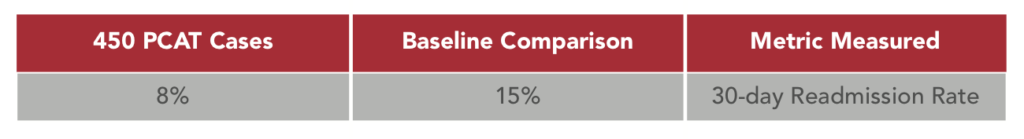
Secondary Impact 2- 30-Day readmission reduction
Simply by performing medication reconciliation up front and instituting more aggressive therapy there was an expectation that the 30-day readmission for patients treated by the PCAT would be lower than their matched baseline comparisons. The results were astounding. Cutting these readmissions by almost half has an enormous impact on the hospital’s reimbursement for services, not to mention patient satisfaction, and, ultimately, patient outcomes.
The PCAT system has a profound impact on organizational efficiency and patient care. There really is no good reason not to do this in every hospital. Also, elements of the PCAT system could be adapted to surgical cases to reduce errors, improve patient management and enhance medication reconciliation – all areas which need improvement.